What you need to know
- COPD is a chronic lung disease, and bronchodilator inhalers are the cornerstone of treatment. Inhaled steroids are added selectively, not used routinely as a first step.
- How you use your inhaler matters as much as which one you take. A surprising number of people get only a partial dose because of small mistakes in technique.
- Smoking cessation, pulmonary rehabilitation, and staying current on vaccines are the non-medication interventions with the strongest evidence behind them.
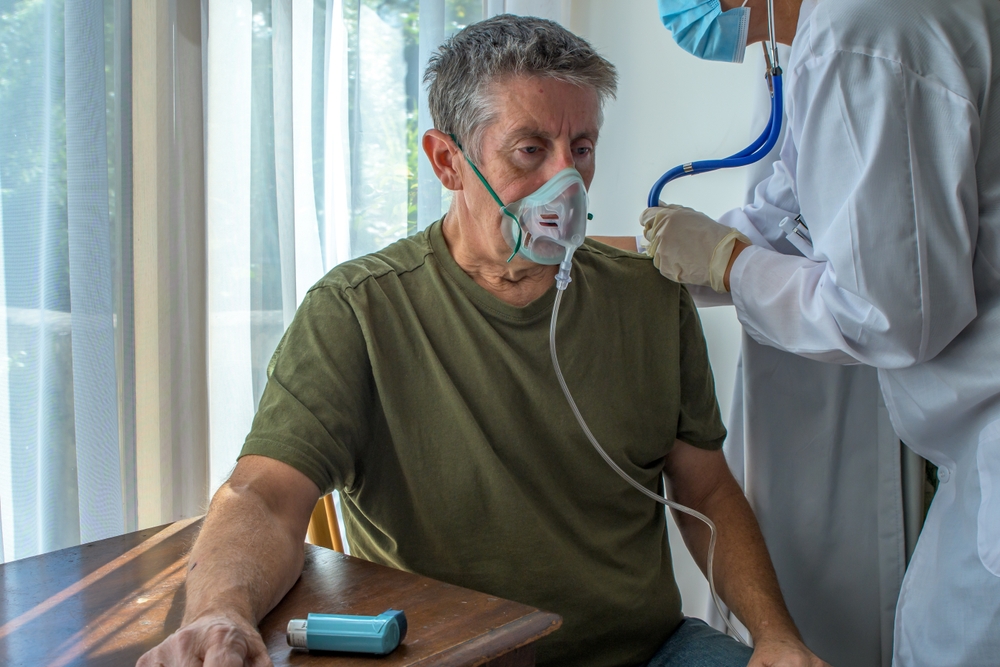
Chronic obstructive pulmonary disease (COPD) is a progressive lung condition that makes it harder to move air in and out of the lungs. It is one of the most common chronic conditions in older adults in the US, and most people who have it manage it with a combination of inhaled medications and lifestyle measures. The medications work — but only if they reach the lungs in the right amounts, which is why inhaler technique is a much bigger part of the picture than it first appears.
COPD shares some features with asthma, and the inhaler categories overlap, but the underlying disease is different and treatment priorities are different too. If you are familiar with the basics from the asthma triggers and management overview, some of what follows will look familiar — but it is worth reading the differences carefully.
How you use your inhaler matters as much as which one you take.
What COPD actually is
COPD is an umbrella term that covers chronic bronchitis (long-term inflammation and mucus production in the airways) and emphysema (damage to the air sacs deep in the lungs). Most cases in the US are linked to long-term smoking, but long-term exposure to dusts, fumes, secondhand smoke, and air pollution also contributes. A smaller share of cases is genetic, linked to a condition called alpha-1 antitrypsin deficiency.
Typical symptoms include shortness of breath (especially with activity), a chronic cough, mucus production, and wheezing or chest tightness. These can build slowly over years. If you have already explored what chest tightness can mean, and your symptoms are recurring or progressive, COPD is one of the conditions a clinician will want to rule in or out — usually with a breathing test called spirometry.
The inhaler menu, simplified
Inhalers fall into a few main categories, and most people end up on more than one over time.
Short-acting bronchodilators (rescue inhalers)
These open the airways quickly and are used as needed for sudden breathlessness. The two main types are short-acting beta-2 agonists like albuterol, and short-acting muscarinic antagonists like ipratropium. Most people with COPD are prescribed a short-acting bronchodilator to keep with them at all times.
Long-acting bronchodilators (maintenance inhalers)
These are taken on a schedule (once or twice a day) to keep the airways open between flare-ups. Long-acting muscarinic antagonists (LAMAs) like tiotropium and umeclidinium, and long-acting beta-2 agonists (LABAs) like salmeterol and formoterol, are the workhorses of long-term COPD treatment. They are often combined into a single inhaler.
Inhaled corticosteroids (ICS)
These reduce airway inflammation. Unlike in asthma, ICS are not first-line for COPD and are usually reserved for people who continue to have flare-ups despite long-acting bronchodilators, or who have certain blood markers (specifically a higher eosinophil count) that suggest steroids will help. They carry a small but real increased risk of pneumonia, which is why they are added selectively rather than by default.
Triple therapy
For people with frequent or severe flare-ups, a single inhaler can deliver all three medication classes (LAMA + LABA + ICS) at once. This is reserved for the more advanced end of the disease.
Why inhaler technique is half the battle
Studies repeatedly find that a large share of people with COPD do not use their inhalers correctly — and incorrect technique means a partial dose. Different inhaler types need different techniques.
- Metered-dose inhalers (MDIs) need a slow, steady breath in, coordinated with pressing the canister. A spacer (a chamber that fits between the inhaler and your mouth) makes this much easier and is recommended for many people.
- Dry powder inhalers (DPIs) need a quick, forceful breath in to pull the powder into the lungs — the opposite of the MDI approach.
- Soft mist inhalers release a slow mist that needs a slow, deep breath, more like an MDI.
Ask your provider or pharmacist to watch you use your inhaler at least once a year. It is one of the highest-leverage things you can do for your COPD, and most people pick up small fixes that meaningfully improve how much medication actually reaches their lungs.
Ask your provider or pharmacist to watch you use your inhaler at least once a year.
Beyond the inhaler
Smoking cessation is the single most effective thing anyone with COPD can do. Quitting slows disease progression more than any medication. If past attempts have not stuck, ask about prescription options — there are several non-nicotine medications that can roughly double the chance of success.
Pulmonary rehabilitation is a structured program of supervised exercise, breathing techniques, and education. It improves exercise tolerance and quality of life, and reduces hospital admissions. Many programs now offer remote or app-based options if getting to a center is difficult.
Vaccines matter more in COPD than they do for the average adult, because respiratory infections can trigger serious flare-ups. Annual flu vaccine, pneumococcal vaccines, COVID-19 boosters, and the RSV vaccine for older adults are typically recommended.
Oxygen therapy is added when blood oxygen levels run consistently low. For severe COPD, supplemental oxygen can prolong life — it is not a sign that things are dire so much as a tool that does what damaged lungs can no longer do alone.
Other medications have a smaller role: short courses of oral steroids and antibiotics during flare-ups, roflumilast for certain people with frequent exacerbations and chronic bronchitis, and a newer add-on biologic approved in 2024 for people whose COPD is not controlled on triple therapy and who have higher eosinophil counts.
When to see a doctor
If you have a long-standing cough, regular shortness of breath with activity, frequent chest infections, or wheezing, get evaluated — particularly if you smoke now or used to. COPD is often diagnosed late, and earlier treatment makes a real difference to long-term lung function.
If you already have COPD, learn the signs of a flare-up (also called an exacerbation): worsening breathlessness, more cough or mucus than usual, change in mucus color (yellow or green), fever, or feeling unusually tired or confused. Flare-ups are often easier to treat early. Seek emergency care for severe shortness of breath, chest pain, blue lips or fingertips, or confusion that comes on quickly — these can signal a medical emergency.
Frequently asked questions
I have several inhalers — how do I keep them straight?
Most people end up with a “rescue” inhaler used only for sudden symptoms, and one or more “maintenance” inhalers taken on a fixed schedule. Ask your pharmacist to label which is which, and consider keeping the rescue inhaler somewhere distinct from the maintenance ones — many people use a different room, a different bag, or a different color cap. If you find yourself reaching for the rescue inhaler more than a couple of times a week, that is a sign your maintenance treatment may need adjusting.
Can I stop my inhalers if I feel fine?
Maintenance inhalers work by keeping inflammation and bronchoconstriction at bay — feeling fine usually means they are doing their job, not that they are no longer needed. Stopping them on your own often leads to a flare-up within weeks. If you would like to reduce or simplify your regimen, this is a real conversation to have with your provider, who can step things down in a controlled way.
Are there pills for COPD, or just inhalers?
Most day-to-day COPD treatment is inhaled, because that delivers medication directly to the lungs with fewer whole-body side effects. But there are oral medications used in specific situations — short courses of steroids and antibiotics during flare-ups, daily roflumilast for certain people with chronic bronchitis and repeated exacerbations, and medications to help with quitting smoking. Inhalers do most of the work; pills fill in around the edges.